Uterine Septum
Embarking on the journey towards parenthood can be both exhilarating and challenging. For some individuals, the presence of a uterine septum can add an extra layer of complexity to this already intricate path. In today’s blog post, we shed light on uterine septum resection—a transformative procedure that paves the way for enhanced fertility and increased chances of a successful pregnancy.
Understanding Uterine Septum:
Before delving into the details of uterine septum resection, it’s essential to grasp the concept of a uterine septum. This structural abnormality involves a dividing wall within the uterus, a condition often present from birth. The implications of a uterine septum extend beyond the physical barrier, influencing fertility and increasing the risk of miscarriage.
Let’s explore the causes and symptoms associated with a uterine septum:
Causes of Uterine Septum:
Congenital Development:
- The primary cause of a uterine septum is a congenital anomaly during fetal development.
- It occurs when the Müllerian ducts, which eventually form the female reproductive organs, do not fuse properly, leading to the development of a septum within the uterus.
Genetic Factors:
- There may be a genetic predisposition to uterine septum, meaning it could run in families.
- Certain genetic mutations or variations may contribute to the development of Müllerian duct anomalies.
Symptoms of Uterine Septum:
Recurrent Miscarriages:
- Women with a uterine septum may experience recurrent miscarriages, especially during the first and second trimesters.
- The septum can interfere with proper implantation of the embryo, leading to pregnancy loss.
Infertility:
- Difficulty conceiving may be a symptom of a uterine septum.
- The septum can hinder the implantation of the fertilized egg or disrupt the normal functioning of the uterus.
Menstrual Irregularities:
- Women with a uterine septum may experience irregular menstrual cycles.
- The septum can affect the normal flow of menstrual blood within the uterus.
Pain or Discomfort:
- Some women with a uterine septum may experience pelvic pain or discomfort.
- This can be associated with the presence of the septum and its impact on the uterine structure.
Obstructed Reproductive Pathways:
- The septum can obstruct the natural pathways for sperm to reach the egg, leading to difficulties in conception.
Abnormal Pap Smear Results:
- In some cases, a uterine septum may be associated with abnormalities in Pap smear results.
- Regular gynecological examinations are essential for detecting such abnormalities.
Preterm Birth:
- Women with a uterine septum may have an increased risk of preterm birth.
- The presence of the septum can affect the ability of the uterus to support a full-term pregnancy.
Diagnosis and Treatment:
Diagnosis:
- Diagnostic tools such as hysterosalpingography (HSG), hysteroscopy, or imaging studies like ultrasound and magnetic resonance imaging (MRI) can help visualize the uterine structure and identify the presence of a septum.
Treatment:
- Uterine septum resection is a common and effective treatment. Surgical procedures, often performed hysteroscopically or laparoscopically, involve the removal or resection of the septum to improve reproductive outcomes.
If you suspect you may have a uterine septum or are experiencing symptoms related to fertility or pregnancy loss, it is essential to consult with a healthcare provider specializing in reproductive health. Early diagnosis and appropriate management can significantly improve the chances of a successful pregnancy.
The Impact on Fertility:

The presence of a uterine septum can hinder the implantation of an embryo or lead to complications during pregnancy. Understanding these challenges is the first step towards finding a solution, and uterine septum resection has emerged as a key intervention in overcoming these obstacles.The septate uterus can impact fertility in several ways:
- Implantation Challenges: The presence of the septum can create difficulties for a fertilized egg to implant properly in the uterine lining.
- Increased Risk of Miscarriage: Women with a septate uterus may have a higher risk of miscarriage, especially during the early stages of pregnancy.
- Obstructed Pathways: The septum can obstruct the natural flow of sperm, hindering their journey to meet an egg for fertilization.
Uterine Septum Resection Unveiled
Diagnosis and Evaluation:
The journey begins with a thorough diagnosis. Advanced imaging techniques, such as hysteroscopy or hysterosalpingography, help healthcare providers visualize the uterine cavity and identify the presence and extent of the septum.
Treatment:
- The Surgical Approach: Uterine septum resection is a surgical procedure aimed at removing the dividing wall within the uterus. This can be achieved through various techniques, including hysteroscopic resection, laparoscopic resection, or a combination of both, depending on the specific characteristics of the septum and the patient’s medical history.
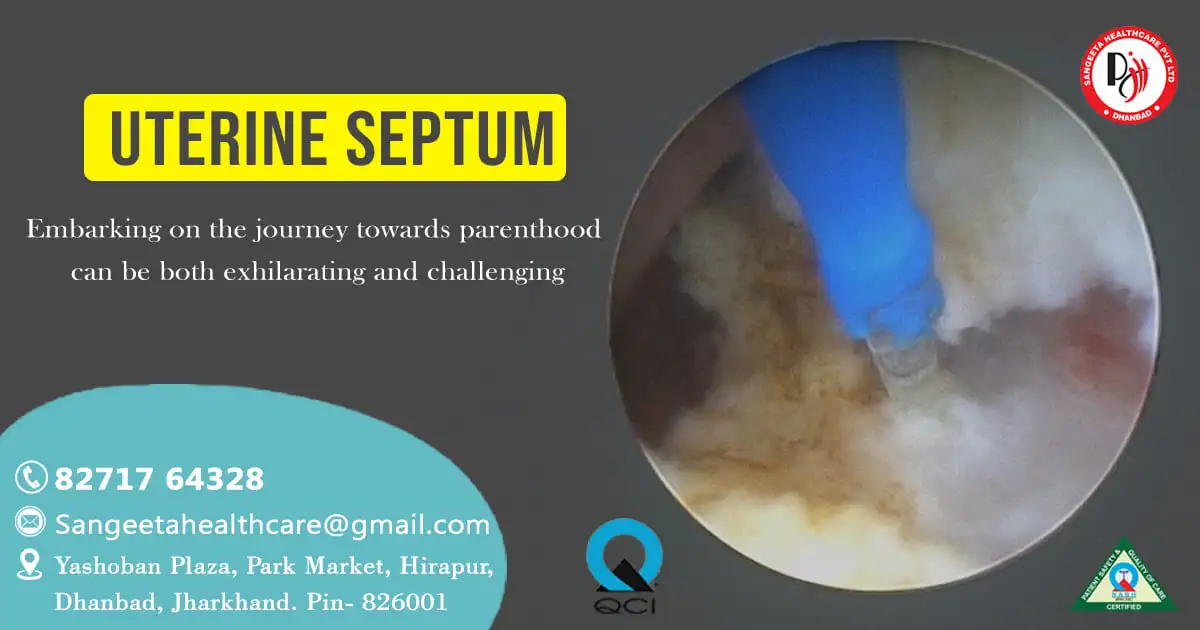
- Hysteroscopic Resection: A hysteroscope, a thin tube with a camera, is gently inserted through the cervix into the uterus, providing a clear view of the septum. Using specialized instruments, surgeons carefully remove the septum, allowing for improved uterine architecture.
- Laparoscopic Resection: In some cases, especially when the septum extends into the muscle of the uterus, laparoscopic techniques may be employed. This involves making small incisions in the abdomen and using a laparoscope to guide the removal of the septum
Laser Therapy in Uterine Septum

Laser technology is one of the tools that may be used in uterine septum resection. The specific type of laser used is often a carbon dioxide (CO2) laser. The laser is used to precisely cut and vaporize tissue, allowing for targeted removal of the uterine septum.
The Laser Advantage:
In the realm of surgical interventions, the utilization of lasers has revolutionized the precision and efficiency of procedures. In the context of uterine septum resection, carbon dioxide (CO2) lasers take center stage. Let’s explore how this advanced technology is transforming the landscape of reproductive surgery.
Precise Visualization with Hysteroscopy:
The journey begins with a hysteroscope, a slender instrument equipped with a camera, carefully inserted through the cervix into the uterus. This allows for real-time visualization of the uterine cavity, enabling surgeons to identify and assess the septum.
Laser Resection Unveiled:
The heart of the procedure lies in the application of laser technology. A carbon dioxide laser, known for its precision and tissue-selective capabilities, is meticulously employed to cut and vaporize the uterine septum. As the laser maneuvers through the tissue, it seals blood vessels, minimizing bleeding and enhancing the safety of the procedure.
Personalized Uterine Cavity Reshaping:
With the laser’s precision, surgeons can tailor the resection to each patient’s unique anatomy. This personalized approach ensures the complete removal of the septum, optimizing the reshaping of the uterine cavity. The goal is to create an environment conducive to improved fertility and reduced pregnancy risks.
Minimized Discomfort and Quicker Recovery:
Laser technology not only aids in precise tissue removal but also contributes to reduced discomfort and faster recovery. The minimally invasive nature of laser-assisted uterine septum resection often translates to shorter hospital stays and a quicker return to normal activities for patients.
Postoperative Guidance and Follow-Up:
As with any surgical procedure, postoperative care is crucial. Patients receive guidance on pain management, antibiotics, and activity restrictions during the recovery period. Follow-up appointments allow for ongoing monitoring, ensuring the success of the procedure and addressing any concerns that may arise.
Uterine septum resection using laser technology stands at the forefront of advancements in reproductive surgery. This precise and personalized approach not only addresses the physical barriers posed by a uterine septum but also opens doors to improved fertility and increased chances of successful pregnancies. As we continue to explore the frontiers of medical innovation, laser-assisted procedures offer hope and possibilities for individuals navigating the intricate path of fertility challenges.The choice of technique will be determined by the surgeon based on individual factors and considerations.
Recovery and Postoperative Care:
Following the procedure, patients are closely monitored for a brief period before being released. Pain management and recovery instructions are provided to ensure a smooth healing process. Most patients can resume their normal activities within a relatively short time frame.
Uterine septum resection offers hope to individuals facing fertility challenges associated with this common uterine anomaly. By addressing the structural impediment within the uterus, this procedure opens doors to improved reproductive outcomes. If you or someone you know is navigating the complexities of fertility and considering uterine septum resection, understanding the procedure’s intricacies is a crucial step towards making informed decisions on the path to parenthood. Remember, breaking barriers is not only a medical procedure but a transformative journey towards building the family you’ve always dreamed of.



 Ectopic Pregnancy
Ectopic Pregnancy









